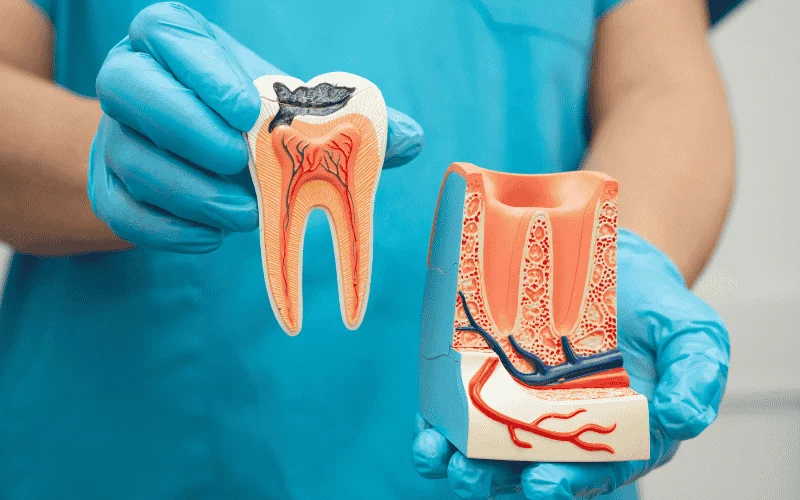
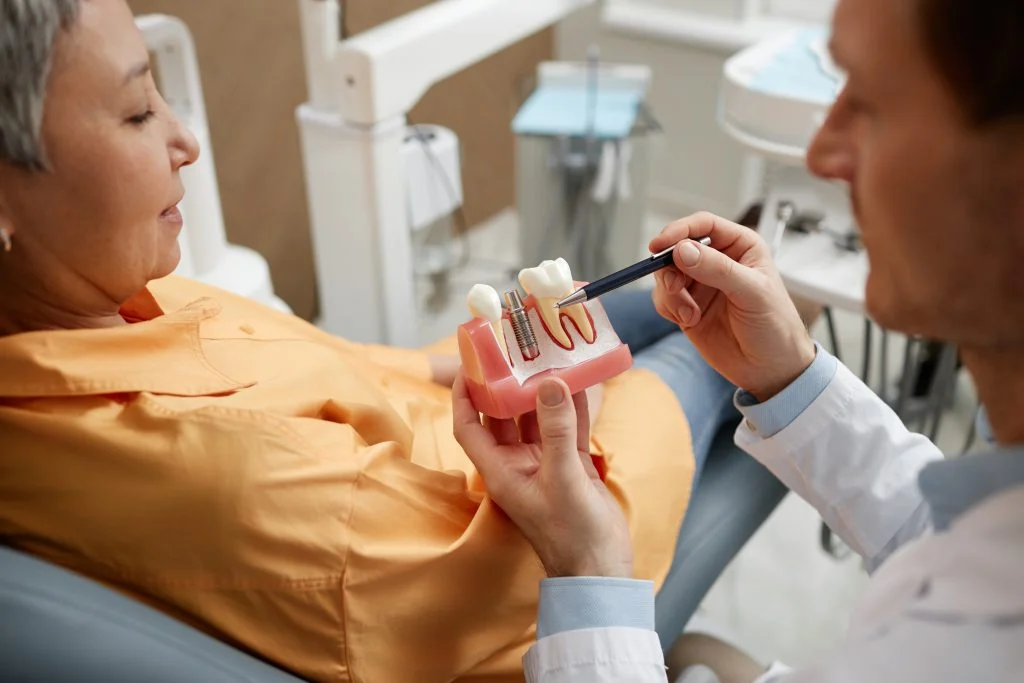
If you have lost a tooth, you may wonder if bone loss will stop you from getting dental implants. Jawbone loss often starts soon after a tooth goes missing because the bone no longer gets pressure from chewing.
Over time, that shrinkage can change how strong and thick your jaw feels.
Dental implants with bone loss can affect your candidacy, but it does not always prevent you from getting them. Implants need enough healthy bone to stay stable, and without it, the risk of failure increases.
Learn more about how bone loss affects dental implant success rates and why a strong foundation matters.
The good news is that modern dentistry offers options if your bone has thinned. Many people still qualify with added procedures or alternative implant methods.
You can also explore whether severe bone loss limits dental implant treatment and what solutions may help in your case.
Key Takeaways
- Healthy jawbone supports strong and stable dental implants.
- Bone loss may require added procedures before implant placement.
- Advanced techniques can help many people qualify for implants.
Book a consultation at Wojtowicz Dental to explore if implants are right for you.
Why Jawbone Health Matters for Dental Implants
Your jawbone does more than hold teeth in place. It provides the base that supports the titanium post, allows osseointegration, and determines how stable your implant will be over time.
How Dental Implants Rely on Jawbone Structure
A dental implant replaces your tooth root with a titanium post. Your dentist places this post directly into your jawbone.
Over the next few months, your bone grows around the post in a process called osseointegration. This bond locks the implant in place. Without it, the implant cannot handle normal biting and chewing forces.
You need enough jawbone height and width to surround the implant. Most dentists look for at least 1–2 mm of healthy bone around the implant to support long-term stability.
If your jawbone is too thin or soft, the implant may shift. Movement can interrupt healing and lower implant success rates. That is why implant dentistry always starts with a close look at your jawbone structure.
Bone Resorption After Tooth Loss
When you lose a tooth, your jawbone stops getting regular pressure from chewing. Without that stimulation, the body begins a process called bone resorption.
Bone resorption means your body breaks down and absorbs bone tissue. This process can start within 3 to 6 months after tooth loss. In the first year, you may lose up to 25% of bone width in that area.
As bone shrinks, your jaw can change shape. You may notice:
- A sunken look in your cheeks
- Loose dentures
- Less space to place an implant
Dental implants help limit this loss because they act like natural tooth roots. They send pressure into the bone when you chew. This stimulation helps preserve jawbone density.
The Impact of Bone Density on Implant Success
Bone density refers to how strong and compact your jawbone is. Dense bone grips the implant firmly and supports better implant stability.
If your bone is too soft, the titanium post may not anchor well. Poor anchoring can delay healing or increase the risk of implant failure. Strong bone improves implant success rates because it supports proper osseointegration.
Your dentist may use 3D imaging to measure jawbone density before surgery. This step helps determine whether you need bone grafting first.
Certain factors can reduce bone density, including:
- Long-term tooth loss
- Gum disease
- Osteoporosis
- Smoking
Understanding the connection between dental implants and jawbone health can help you see why a healthy, dense jawbone gives your implant the best chance to last for many years.
Visit Wojtowicz Dental for a detailed assessment on how bone loss impacts implant treatment options.
Causes and Risk Factors for Bone Loss
Bone loss in your jaw often starts with tooth loss, gum infection, or health issues that affect bone strength. When you understand these risks, you can act early and protect your dental implant options.
Tooth Loss and Missing Teeth
When you lose a tooth, you also lose the root that stimulates your jawbone. Chewing sends signals through the root that keep bone tissue active. Without that pressure, your body begins a process called resorption.
Research shows you can lose up to 25% of bone density in the first year after losing a tooth. This loss can happen faster than most people expect.
If you leave missing teeth untreated, nearby teeth may shift. That movement can change how your bite works and place uneven force on your jaw. Over time, this can increase dental bone loss in certain areas.
Replacing missing teeth early helps protect bone and keeps more implant options open.
Periodontal Disease and Gum Health
Periodontal disease is one of the most common causes of dental bone loss. It starts as gum inflammation but can progress into periodontitis, which damages the bone that supports your teeth.
Bacteria build up along the gumline when oral hygiene slips. If you do not remove plaque each day, your gums can pull away from your teeth and form pockets. These pockets trap more bacteria and deepen the infection.
As periodontitis advances, your body breaks down bone around the teeth. This damage can make teeth loose or lead to tooth loss.
You lower your risk by brushing twice daily, flossing, and keeping regular dental visits. Early treatment of gum disease can slow or stop further bone damage.
Medical and Lifestyle Contributors
Some health conditions weaken bone throughout your body, including your jaw. Osteoporosis reduces bone density and may affect how well bone supports teeth or integrates with implants.
Other systemic and local risks also play a role. Reviews of risks and complications associated with dental implant failure describe how smoking, uncontrolled diabetes, and poor healing can affect bone stability.
Smoking limits blood flow to your gums. Diabetes can slow healing and raise infection risk. Both can increase dental bone loss over time.
Your daily habits matter. Poor oral hygiene allows bacteria to thrive, while balanced nutrition supports bone health.
When you manage medical conditions and avoid tobacco, you protect your jawbone and improve your chances of qualifying for dental implants.
Learn more about implants to see why it works best for your bone health and smile.
How Bone Loss Influences Dental Implant Candidacy
Bone loss changes how your dentist plans implant placement. Your jaw must have enough height, width, and strength to hold dental implants in place for years.
Assessing Bone Quantity and Quality
Your dentist checks both the amount of bone and the strength of that bone before placing an implant.
They often use digital X-rays and a cone beam CT scan (CBCT) to get clear images of your jaw. A cone beam CT scan provides 3D imaging that shows bone width, height, and density.
This detail helps your dentist measure exactly how much bone supports the implant site.
Bone quantity refers to how much jawbone remains after tooth loss. When you lose a tooth, the area no longer gets pressure from chewing. Over time, this can lead to jawbone loss.
Bone quality refers to density and strength. Softer bone may not hold an implant as firmly, even if there seems to be enough volume. Your dentist uses this data to decide if you need bone grafting before implant placement.
Areas Most Affected by Bone Loss
Bone loss does not affect every part of your jaw the same way.
The upper back jaw often loses bone faster, especially near the sinus cavity. In this area, limited bone height may require a sinus lift before implant placement.
The lower back jaw can also lose width over time, which may limit standard dental implants.
Long-term tooth loss and advanced gum disease increase the risk of jawbone loss in these areas.
Your dentist uses 3D imaging to map these high-risk zones. This planning helps protect nearby nerves and sinus spaces while improving implant stability.
Potential Complications Including Implant Failure
If you have significant bone loss, the biggest concern is dental implant failure.
An implant must fuse with your jaw in a process called osseointegration. Without strong bone health, the implant may not bond correctly. This can lead to loosening, discomfort, or implant failure.
Research on factors affecting bone around implants shows that early bone loss can increase the risk of problems over time, including bone loss in dental implants during the first year after placement.
Other risks include:
- Poor initial stability
- Increased stress on surrounding bone
- Inflammation around the implant
Careful planning with CBCT scans and proper treatment before implant placement lowers these risks. When your dentist addresses bone concerns early, you improve your chances of long-term success.
Restoring Candidacy: Advanced Techniques and Solutions
You can often qualify for implant treatment even after bone loss. Dentists use targeted procedures to rebuild bone, add support in thin areas, or place implants in stronger parts of your jaw.
Bone Grafting Procedures
A bone graft rebuilds areas where your jaw has thinned or shrunk. Your surgeon places grafting material in the weak spot to support future implants.
Over time, your body replaces this material through natural bone regeneration.
You may receive an autograft, which uses bone from your own body. Other options include donor or synthetic materials. Each type supports healing in a slightly different way, but all aim to create a stable base for implants.
Many providers use guided bone regeneration during bone grafting procedures.
This method places a special membrane over the graft to protect it and guide new growth. Healing often takes a few months before your implant treatment can move forward.
Sinus Lift and Ridge Augmentation
If you need implants in your upper back jaw, you may not have enough bone below the sinus cavity.
A sinus lift procedure adds bone to this area. Your surgeon gently raises the sinus membrane and places graft material underneath.
After healing, the new bone can support standard implants. Many patients who were once told they lacked enough upper jaw bone can move forward with care.
Ridge augmentation focuses on the shape and width of your jaw ridge. If the ridge is too narrow, your surgeon adds graft material to widen it. This creates better support and improves implant position.
Mini and Angled Implants
In some cases, your dentist may recommend mini implants instead of standard ones. Mini implants are thinner and can fit in areas with limited bone. They often require less invasive surgery and may involve shorter healing times.
Angled implants offer another solution. Instead of placing the implant straight down, your surgeon tilts it to anchor into stronger bone. This approach can avoid the need for certain grafting procedures.
These options help you move forward with implant treatment even if bone loss limits traditional placement. Your provider will study your scans and choose the method that gives you stable, long-term support.
Implant Options for Severe or Complex Bone Loss
Severe bone loss does not always rule out dental implants. You still have options, including special implant designs and prosthetics that work around weak or missing jawbone.
Zygomatic Dental Implants and Zygoma Techniques
If you have severe bone loss in the upper jaw, standard implants may not hold well. In this case, your surgeon may recommend zygomatic dental implants.
These implants anchor into the zygoma, or cheekbone, instead of the upper jawbone. The cheekbone is dense and strong, which gives the implant solid support even when upper jaw bone loss is advanced.
Unlike traditional implants, zygomatic implants are longer and require special training to place. They often help you avoid large bone graft procedures.
You may qualify for this option if you:
- Have severe upper jaw bone loss
- Want to avoid sinus lifts or major grafting
- Need a full upper arch restoration
Implant-Supported Dentures and Bridges
If you still have some healthy bone, you may not need advanced implants. Implant-supported dentures or implant-supported dental bridges can restore function with fewer implants.
Your dentist places a small number of implants in areas with enough bone.
These implants support a full arch denture or bridge. This approach spreads pressure across multiple implants, which improves stability.
Compared to traditional dentures, implant-supported dentures:
- Do not slip as easily
- Improve chewing strength
- Help reduce further bone shrinkage
If bone levels are moderate, you may still qualify for treatment.
Partial dentures can also attach to implants for added stability when you are missing only a few teeth.
Alternative Tooth Replacement Solutions
If implants are not safe due to health issues or very severe bone loss, you still have choices.
Traditional dentures rest on your gums and do not require surgery. They cost less upfront, but they do not stop bone shrinkage. Over time, you may need relines or replacements as your jaw shape changes.
Partial dentures replace several missing teeth and use clasps to attach to natural teeth. They work well when you still have healthy teeth for support.
Dental bridges use nearby teeth as anchors instead of implants. Your dentist reshapes those teeth to hold the bridge in place. This option avoids surgery but does not prevent bone loss under the missing tooth.
Your dentist will review your bone levels, overall health, and goals before recommending the right path for you.
Personalized Treatment Planning and Long-Term Success
Your results depend on careful diagnosis, skilled placement, and steady follow‑up care. When you and your provider focus on these steps, you improve your chances of stable implants and healthy bone for years.
Comprehensive Diagnosis and Imaging
You need more than a quick exam to know if implants will work. Your provider should review your medical history, check your gums, and measure bone levels.
Advanced 3D imaging plays a key role. A detailed 3D scan for implant planning shows bone height, width, and density. Many offices use cone beam CT to see nerves, sinuses, and thin bone areas before surgery.
This data shapes your customized treatment plan. Your provider can decide if you need bone grafting, extra implants for support, or a staged approach with longer healing time.
Clear imaging also lowers risk. It helps your team place implants at the right angle and depth, which supports long-term stability.
Role of the Implant Specialist
An experienced implant specialist or oral surgeon understands how bone quality affects stability. This matters even more if you have moderate or severe bone loss.
Specialists focus on precise treatment planning. They decide implant size, position, and number based on your anatomy, not a one‑size‑fits‑all model.
In complex cases, they may suggest options such as grafting or alternative implant types. Some patients with limited bone may qualify for alternative implant solutions for limited jawbone instead of traditional implants.
Working with a trained provider protects your investment. It also gives you realistic expectations about healing time and the steps needed to restore your smile safely.
Maintaining Jawbone and Implant Health
Your job does not end after surgery. Daily care and routine visits protect both your implants and your jawbone.
Brush and floss around implants just as you would natural teeth. Your dentist may recommend special brushes or tools to clean under the restoration.
Regular checkups allow your provider to monitor bone levels and watch for peri-implantitis, an infection that can damage bone around implants. Early treatment can prevent serious problems.
Implants also help support bone by replacing the tooth root. Dental implants help prevent bone loss long term by stimulating the jaw.
When you follow your care plan and attend maintenance visits, you give yourself the best chance to restore your smile and keep it strong.
Frequently Asked Questions
Bone loss can affect implant stability, treatment cost, and your choice of procedures. You still have options, even if your jawbone has weakened over time.
What can cause bone loss around existing dental implants?
Bone loss around an implant often starts with peri-implantitis. This is an infection of the gum and bone around the implant.
Poor oral hygiene, smoking, and uncontrolled diabetes raise your risk. Too much bite pressure or a poorly placed implant can also strain the bone.
If you skip cleanings, plaque can build up and lead to inflammation. Over time, that inflammation can break down the bone that holds your implant in place.
How does bone loss impact the cost of dental implants?
Bone loss can increase your total cost because you may need extra procedures. Bone grafting, sinus lifts, or advanced imaging add to the treatment plan.
For example, treatment plans that include grafting or other added steps often cost more than standard placement.
More complex cases also take more visits and longer healing time. That can raise both clinical and personal costs, such as time off work.
Are there signs that indicate bone loss has affected my dental implant?
You may notice your implant feels loose. Healthy implants should not move.
Red, swollen, or bleeding gums around the implant can also signal trouble. Bad breath or a bad taste that does not go away may point to infection.
Your dentist may see bone changes on X-rays before you feel symptoms. Regular checkups help catch problems early.
Is it possible to receive dental implants if I currently have bone loss?
Yes, in many cases you can still get implants. Modern methods allow dentists to work around mild to even severe bone loss.
Your dentist will review your medical history, take 3D scans, and measure bone volume. That information guides your plan.
What options exist for patients with insufficient bone mass for dental implants?
Bone grafting can rebuild areas where bone has thinned. Your body slowly replaces the graft material with new bone.
Mini implants may work in narrow spaces with less bone. Implant-supported dentures can also reduce the number of implants you need.
Some patients benefit from sinus lifts in the upper jaw. Each option depends on how much bone you have and where the loss occurred.
How do zygomatic implants differ from standard dental implants for patients with bone loss?
Standard implants anchor into your jawbone. They need enough height and width for support.
Zygomatic implants anchor into your cheekbone instead of your upper jaw. This approach helps when you have severe bone loss in the upper jaw.
Zygomatic implants are longer than standard implants. They often reduce the need for large bone grafts in the upper jaw.